Difference between Brain Death, Coma and Vegetative State
Brain death is often confused with other seemingly similar conditions, such as coma and vegetative state. The characteristics of each condition are described below.
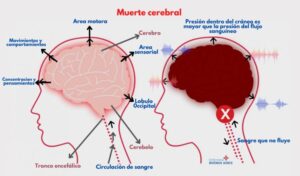
Brain death
Brain death is the irreversible cessation of all brain functions, including the brainstem. A brain-dead person is dead, with no possibility of revival. Once the brain tissue dies, no treatment is possible.
Brain death is death. There is no brain function. Brain death results from swelling of the brain; blood flow in the brain ceases and without blood to oxygenate the cells, the tissue dies. It is irreversible.
The brain performs many functions, including thinking, movement, and all the neurological functions that allow the body to maintain blood pressure, heart rate, body temperature, breathing, etc.; in constant balance. When a patient deteriorates to brain death, the entire body system shuts down; he can’t breathe, his heart can’t beat, and his body can’t function once his brain dies. Massive artificial medical measures to maintain organ function (such as mechanical ventilation support) must be initiated, but these interventions are only a temporary measure.
Causes of brain death
The causes of brain death occur when the supply of blood and/or oxygen to the brain is stopped and they are:
- Cardiac arrest: the heart stops beating and the brain runs out of oxygen.
- Heart attack: The blood supply to the heart is suddenly blocked.
- Stroke: The blood supply to the brain is blocked or interrupted.
- Blood clot: Blockage in a blood vessel that disturbs or blocks the flow of blood around the body.
- Serious head injury.
- Cerebral haemorrhage.
- Brain infection: encephalitis.
- Brain tumor.
Signs of brain death
Some of the signs of brain death are:
- Electroencephalogram: does not show any brain activity.
- Pupils: Pupils are unresponsive to light and fixed, without oculocephalic reflexes.
- Pain: the patient shows no reaction to pain; example: if the body is pinched; does not frown or move any limbs.
- Eyes: the eyes do not blink when the surface of the eye is touched (corneal reflex); they do not move when the head is turned (oculocephalic reflex) and they do not move when ice water is poured into the ear (oculovestibular reflex).
- The gag reflex disappears: when the back of the throat is touched; the patient does not have the reflex to vomit.
- Ventilator Off: Patient is not breathing when the ventilator or ventilator is off; there is no spontaneous breathing.
Diagnosis of brain death
Tests performed to determine if brain death has occurred; they are tests that confirm that the patient does not respond to verbal or visual command, the patient is flaccid; the pupils do not react and are fixed; no oculocephalic, gag, oculovestibular, or corneal reflexes; and there is no spontaneous breathing.
Even after confirmation of these tests, additional tests are performed before pronouncing brain death. These tests include: electroencephalogram (EEG) and the study of cerebral blood flow (CBF).
Electroencephalogram (EEG)
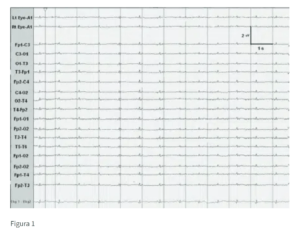
The EEG measures brain voltage in microvolts. It is so sensitive that static electricity on a person’s clothing will give a squiggle on the EEG (a false positive). All positive responses suggest brain function. The patient in the deepest coma will show some EEG electroactivity, while the brain-dead patient will not.
Figure 1: Electrocerebral silence in a brain-dead patient by digital electroencephalogram (EEG).
Cerebral blood flow (CBF) study
The study of cerebral blood flow (CBF) involves the injection of a mild radioactive isotope into the bloodstream. By placing a radioactivity counter on the head, the amount of blood reaching the brain can be measured. If there is no blood flow to the brain, the brain is dead. A negative cerebral blood flow study is indisputable evidence of a dead brain. See figure 2.
Only after brain death has been confirmed and the time of death noted can organ donation become a possibility.
Coma
Coma is a state of profound unresponsiveness resulting from serious illness or brain injury. Coma patients do not open their eyes or speak, and do not exhibit purposeful behavior.
Some patients require ventilator support; while others don’t. Intensivists all too often put patients in medically induced comas to give the brain time to heal. Usually; the coma may last only a few days or weeks.
A patient in a coma is a living patient and has some brain activity. The comatose patient may have brainstem responses, spontaneous breathing, and/or purposeless motor responses. The coma has 3 possible outcomes and they are:
- Recovery of consciousness.
- Evolution to a state of chronically depressed consciousness: vegetative state.
- Progression to brain death.
Depending on the severity of the brain injury; recovery time varies and comas can be temporary or permanent. Coma patients are not considered for organ, eye or tissue donation.
Causes of coma
Coma can be natural or induced. Natural coma is caused by injury to the brain. And an induced coma is caused by an intensivist doctor when the patient is under mechanical ventilation, for example. Some of the causes that can lead a patient to a natural coma are:
- Traumatic brain injury.
- Stroke or seizure.
- Brain tumor.
- Infections involving the brain
- Brain damage caused by a prolonged lack of oxygen.
- Overdose of medication or other drugs.
- Chemical imbalances caused by an underlying disease.
Coma signs
Signs of coma usually include the following:
- Closed eyes.
- Weakened brainstem reflexes: pupils that do not respond to light.
- Unresponsive extremities: except reflex movements.
- Pain: there is no response to painful stimuli, except reflex movements.
- Irregular breathing.
Coma diagnosis
To identify that a patient is in a coma; certain exhaustive tests are required. This often involves three types of tests: physical exam, lab tests, and brain scans.
The physical exam checks:
- Reflexes.
- Response to pain.
- Vocal noises.
- Observing eye reactions: Doctors may spray cold water into the patient’s ear canal and monitor eye movement or a reflex response.
Laboratory tests look in the blood for the status of:
- Glucose.
- Liver and kidney function.
- Carbon monoxide poisoning.
- Drugs or alcohol.
A lumbar puncture may also be done to find infections in the nervous system.
The brain scan consists of images of the brain to help identify areas of injury by:
- CT scan: Provides a detailed image of the brain.
- MRI: used to check for tissue damage.
- EEG (Electroencephalogram): detects activity in the brain.
Vegetative state
The vegetative state occurs when the patient has lost higher brain functions, but their brainstem is intact, allowing essential functions such as heart rate and breathing to continue. A person in a vegetative state is alive and can recover over time.
Causes of the vegetative state
- Relentless progression of degenerative or metabolic neurological diseases.
- Developmental malformations of the nervous system.
Signs of vegetative state
In the vegetative state the patient’s signs are:
- Depressed conscience.
- Depressed brainstem function.
- Unassisted breathing (without mechanical ventilation support).
- Response to pain or loud sounds.
- Sleep and wake cycles.
- Involuntary movements.
A patient is considered in a vegetative state when their condition has been in a permanent vegetative state for more than one year.
Diagnosis of the vegetative state
The vegetative state can be diagnosed according to the following criteria:
- Awareness: The patient is not aware of himself or the environment.
- Interaction: inability to interact with others.
- Visual, auditory, tactile, or noxious stimuli: No evidence of sustained, reproducible, intentional, or voluntary behavioral responses to visual, auditory, tactile, or noxious stimuli.
- Language: no evidence of understanding or expression of language.
- Intermittent wakefulness: it is manifested by the presence of sleep-wake cycles.
- Brainstem and hypothalamic autonomic functions: Sufficiently preserved to allow survival with medical and nursing care.
- Incontinence: bowel and bladder.
- Cranial nerve reflexes: variably preserved (pupillary, oculocephalic, corneal, vestibulo-ocular, and gag).
- Spinal reflexes.
Differences between persistent and permanent
The vegetative state can be persistent or permanent; The difference between these two are very extreme. Despite Jennett and Plum’s precise use of language¹, confusion has arisen about the exact meaning of the term «persistent». The adjective «persistent» refers only to a disabling condition that is past and continues into an uncertain future, while «permanent» implies irreversibility.
Persistent vegetative state is diagnostic and permanent vegetative state is prognostic. Then:
- Persistent vegetative state: Originally defined by Jennett and Plum in 1972, the term “persistent” means sustained over time.
- Permanent vegetative state: “permanent” means irreversible.
Author information
Sources consulted
- Jennett B, Plum F; 1994, Estado vegetativo persistente después del daño cerebral: un síndrome en busca de un nombre. Lanceta 1972 ;1: 734 – 737. Disponible en: https://www.nejm.org/doi/pdf/10.1056/NEJM199405263302107?articleTools=true
- R. Berkow, M. Beers, A. Fletcher & R. Bogin, 2015, Stupor and coma – general [en línea], The Merck Manual of Diagnosis and Therapy, Merck & Co., Inc., Whitehouse Station, Nueva Jersey, EE. UU. Disponible en: https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/brain-death
Last update: [ 09/17/2022 ]