Breathing frequency
The respiratory cycle includes an inspiration phase and an expiration phase. Respiratory rate (RR) is the number of times a person breathes per minute. It is recommended to carry out the RF control when the person is at rest and without being aware that we are controlling the RF; (so that in this way your breathing is natural). The RR assessment consists of counting the number of breaths for one minute (1 minute) visualizing the number of times the chest rises.
Normal values
The normal respiratory rate (RR) in an adult at rest is between 15 and 20 cycles per minute; that is, 15 x′ to 20 x′. When the RR at rest is greater than 25 x’ breaths per minute or less than 12 x’, it can be considered abnormal.
Respiratory Rate Characteristics
- Ventilation: when breathing; The body takes oxygen from the ambient air into the alveoli and expels carbon dioxide, this is achieved through ventilation or the mechanical process of mobilizing air.
- Presence of respiration: presence of respiration or RF is observed when air enters through chest expansion and when air leaves through chest depression.
- Inspiration: active phase. It is due to contraction of the diaphragm and intercostal muscles. In pathological conditions, the accessory muscles of inspiration are involved: scalenus and sternocleidomastoid.
- Expiration: passive phase. It depends on the lung elasticity. In pathological conditions, the accessory muscles of expiration are involved – the abdominal muscles.
- Rhythm: (regular or irregular). The respiratory rhythm can be regular and irregular, within the irregular rhythm breaths are: Kussmaul, Biot and Cheyne-Stoques breathing.
- Depth: (shallow or deep), the respiratory depth varies according to sex (greater in men than in women), age, height and body position.
- Lung volume: Volume current or current: it is the amount of air that enters and leaves in each normal breath, in an adult it is approximately 500cc, in women it is 20/25 less.
- Inspiratory reserve volume: volume of additional air that can be inspired above the tidal volume, it ranges between 3000 ml and 3500 ml.
- Expiratory reserve volume: volume that can be forcefully expired, after tidal or tidal volume, ranges from 100 to 1200 ml.
- Residual Volume: amount of air remaining in the lungs after expiration of tidal and reserve volumes.
- Affected RF: RF can be affected by the anatomical properties of the chest wall, chest cavity, and upper and lower airways.
- Involuntary Breathing: Involuntary breathing is controlled by the medulla oblongata.
- Organs involved in RF: in breathing, in addition to the organs of the respiratory system, the different structures of the rib cage are involved.
- Total lung capacity: corresponds to the total sum of the lung volumes, it is approximately 5,700/6,200 ml.
Technique for taking the respiratory rate
- Verify the patient’s identity and respect their privacy.
- Place the patient as comfortably as possible sitting or lying down, in the semi-Fowler’s position, but allowing the respiratory rate to be counted. Keep in mind that the poor alignment of the body prevents the correct expansion of the chest and decreases ventilation, therefore; It influences the respiratory rate and volume.
- Monitor (by looking and counting) chest movements without alerting the patient. It is advisable not to inform the patient that the respiratory rate is to be measured, as this could inadvertently change the rhythm.
- It is recommended to measure RF at the same time as monitoring other vital signs, eg (pulse).
- Count up to 30” and multiply this value by 2; provided the breathing is regular.
- In patients with irregular breathing, monitor for 1 minute or longer if necessary.
- Observe respiratory movements, count elevations (inspirations) of the chest and/or abdomen for 1 minute.
- Place one hand on the patient’s chest to feel the respiratory movements. Count inspirations for 1 minute.
- Auscultation: Place the stethoscope on the chest and count the number of inspirations for 1 minute.
- Young children: quantify the upward and downward movements of the abdomen (diaphragmatic breathing).
- Observe the rhythm (regular or irregular), depth and volume (shallow or deep) and characteristics of respiration, also the coloration of skin and nails and use of accessory muscles.
- Disinfect the stethoscope head, after use and between patients.
- Perform hand hygiene, according to procedure.
- Record the data evaluated in the nursing report. Write the nurse’s full name, date, time, registration number and signature.
There is also the auscultatory and palpatory method (or combining inspection, palpation and auscultation).
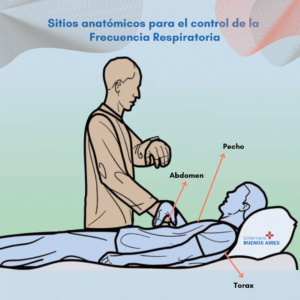
Places to take the FR
The most common places to take the RF are:
- Chest.
- Thorax
- Abdomen.
Purpose of measuring respiratory rate
The main objective of RF measurement is to rule out any physiological alteration in people with or without previous pathologies. RR monitoring is used to determine if the respiratory rate is normal (eupnea).
Changes in respiratory rate
Alterations in the respiratory pattern and rhythm are:
- Bradypnea: it is the slowness in the respiratory rate with an RR of less than 12 x’ breaths per minute. It can be found in patients with neurological or electrolyte disorders, respiratory infection or pleurisy.
- Tachypnea: RR persistently greater than 20 x’; It is a shallow and rapid breath. It is observed in anxious patients, with pain due to rib fracture or pleurisy, in exercise and in CNS disorders.
- Apnea: is the absence of respiratory movements. It is usually a serious condition.
- Dyspnea: subjective sensation of the patient with an effort to breathe. It can be inspiratory, expiratory or both phases.
- Inspiratory dyspnea: it is caused by partial obstruction of the upper airway and is accompanied by retractions, it is usually related to acute processes.
- Respiratory dyspnea: it is associated with narrowing of the lumen of the bronchioles and expiration is prolonged as in patients with bronchial asthma and pulmonary emphysema, this dyspnea is associated with chronic conditions.
- Retractions: indicate obstruction to inspiration; the accessory muscles of inspiration are activated, creating more traction on the chest wall.
- Orthopnea: this is the inability to breathe easily in a recumbent position.
- Kussmaul breathing: RR greater than 20 x’ per minute, deep, sighing and without pauses. It occurs in patients with renal insufficiency and metabolic acidosis.
- Cheyne-Stokes respiration: hyperpnea that is combined with intervals of apnea. In children this pattern may be normal. In adults, it presents as bilateral lesions of the cerebral hemispheres, basal ganglia, medulla oblongata, pons, and cerebellum.
- Biot’s respiration: characterized by extreme irregularity in the rate, rhythm, and depth of respirations.
There are periods of apnea. It is seen in meningitis and other serious neurological injuries.
The last 3 abnormal respiratory patterns (9,10,11) are indicative of severe clinical conditions and poor prognosis. The increase in RF has been related to the severity of septic states, so early identification of this allows more timely and aggressive actions that can improve the prognosis of patients.
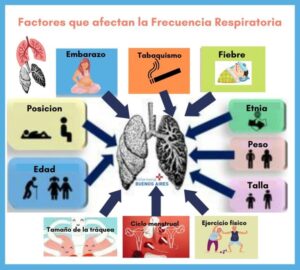
Variables Affecting RF
- Sex (greater in men than in women): standard morphometric methods confirm that men have larger lungs than women and, consequently, a greater number of bronchi, greater alveolar surface area, and larger diameter of the airways. wide, considering subjects of the same weight and height
- Age: lung maturity is reached approximately at 20-25 years, from which a progressive deterioration of lung function begins
- Stature: tall individual and, therefore, with a large lung capacity; will suffer a greater decrease in their lung volumes with increasing age compared to people with shorter stature
- Weight gain.
- Body position: in the vertical position, the lung volumes are greater than in the other positions due to the increased volume of the thoracic cavity.
- Pregnancy.
- Menstrual cycle.
- Chest diameter.
- Trachea size: The diameter of the trachea is smaller in women.
- Physical activity level.
- Of smoking.
- Pathologies.
- Fever: RF can increase with fever and other medical conditions.
Author Information
- Plazas Lorena. Lic. en Enfermería. trabajo propio
Sources consulted
- Fundación Británica del Corazón, 2022, Escocia. Disponible en: https://www.bhf.org.uk/informationsupport/how-a-healthy-heart-works/your-heart-rate
- Villegas González, Juliana; Villegas Arenas, Óscar; Semiología de los signos vitales: Una mirada novedosa a un problema vigente, Archivos de Medicina (Col), vol. 12, núm. 2, julio-diciembre, 2012, pp. 221-240, Universidad de Manizales, Caldas, Colombia. Disponible en: https://www.redalyc.org/pdf/2738/273825390009.pdf
- JS Wanger, BH Culver, 2016, Estándares de calidad en las pruebas de función pulmonar: Pasado, presente, futuro. Ann Am Thorac Soc, 13 (2016), pp. 1435-1436, Disponible en: http://dx.doi.org/10.1513/AnnalsATS.201604-300ED | Medline